It’s clear we’ve entered a new age of medical testing. Whereas in previous generations, testing for disease and genetic conditions seemed nearly impossible, we’ve managed to develop relatively easy, innovative, and effective ways doing just that, with surprising accuracy. Case and point: scientists may be able to determine a person’s […]
Posts archive for July, 2015
What You Don’t Know Acid Reflux and Antacids
Chances are you’re no stranger to the stresses of daily life. Because of it, many of us may be accustomed to that burning sensation in our chests that we may have come to associate with stress. But is heartburn really caused by stress? Antacids are seemingly a quick and easy […]
Walking Off Depression – Looking to Nature to Improve Within
It’s no secret that we could all probably benefit from going outside and getting some fresh air from time to time. Unfortunately, as we get older, we often grow more sedentary. Many of us may become residents of our couches and living rooms. But new studies show that regular access […]
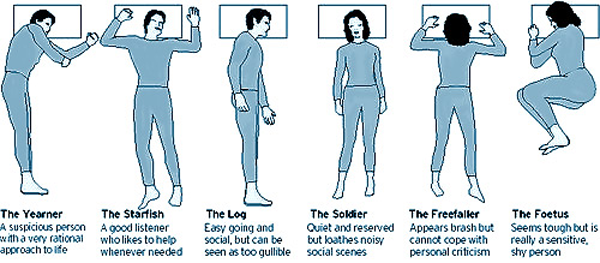
How Sleep Position Effects Personality
Ah, sleep. Seldom do we get enough. According to the Center for Disease Control and Prevention, or CDC, sleep disorders are a national public health epidemic. Adults who get insufficient amounts of sleep are statistically more likely to suffer from motor vehicle crashes, industrial disasters, and medical and other occupational […]